Discover Current Gender-Affirming Care Guidelines: Comprehensive Protocols and Best Practices
Gender-affirming care is a critical aspect of healthcare for transgender individuals, encompassing a range of medical, psychological, and social support services. This article aims to provide a comprehensive overview of the current guidelines and best practices in gender-affirming care, focusing on the latest clinical standards, hormone therapy protocols, surgical interventions, mental health support, and legal considerations. As the landscape of transgender healthcare evolves, it is essential for healthcare providers to stay informed about the most effective and evidence-based practices. This guide will explore the latest updates in clinical guidelines, the administration of hormone therapy, surgical options available, the integration of mental health support, and the legal and insurance challenges that may affect access to care. By understanding these components, healthcare professionals can better support their patients in navigating their gender-affirming journeys.
Research consistently affirms the effectiveness of these interventions in treating gender dysphoria.
Efficacious Gender-Affirming Treatments: Hormones & Surgery
Gender-affirming care, including hormone therapy, “top” (e.g., chest reconstruction surgery) and “bottom” (e.g., vaginoplasty, phalloplasty, metoidioplasty, etc.) surgeries, and puberty blockers, is an efficacious treatment of gender dysphoria for transgender and gender nonconforming (TGNC) individuals.
Barriers to gender-affirming care for transgender and gender nonconforming individuals, JA Puckett, 2018
What Are the Latest Clinical Guidelines for Gender-Affirming Care?
The latest clinical guidelines for gender-affirming care are primarily informed by the World Professional Association for Transgender Health (WPATH) standards, which emphasize the importance of individualized care and informed consent. These guidelines advocate for a holistic approach to transgender healthcare, ensuring that patients receive comprehensive support tailored to their unique needs. Recent updates have highlighted the significance of evidence-based practices in treatment protocols, aiming to improve patient outcomes and satisfaction.
These comprehensive guidelines often include specific training topics to ensure culturally competent and effective care.
Clinical Guidelines for Gender-Affirming Primary Care
As discussed in this review, training topics may include TNG health issues and cultural competency, gender-affirming care, collection and use of gender identity, and confidentiality.
A review of clinical guidelines for creating a gender-affirming primary care practice, 2020
How Do WPATH Standards Define Transgender Healthcare Protocols?
WPATH standards serve as a foundational framework for transgender healthcare, outlining essential protocols for assessment, treatment, and follow-up care. These standards emphasize the importance of informed consent, ensuring that patients are fully aware of their treatment options and potential outcomes. Additionally, WPATH encourages a multidisciplinary approach, integrating medical, psychological, and social support to address the diverse needs of transgender individuals.
What Updates Have Been Made in 2022-2023 Gender Dysphoria Treatment Standards?
The updates to the gender dysphoria treatment standards from 2022 to 2023 reflect a growing recognition of the need for personalized care. Key updates include expanded eligibility criteria for hormone therapy and surgical interventions, as well as enhanced guidelines for mental health support. These changes aim to reduce barriers to care and ensure that all individuals seeking gender-affirming treatment can access the services they need.
How Is Affirming Hormone Therapy Administered Safely and Effectively?
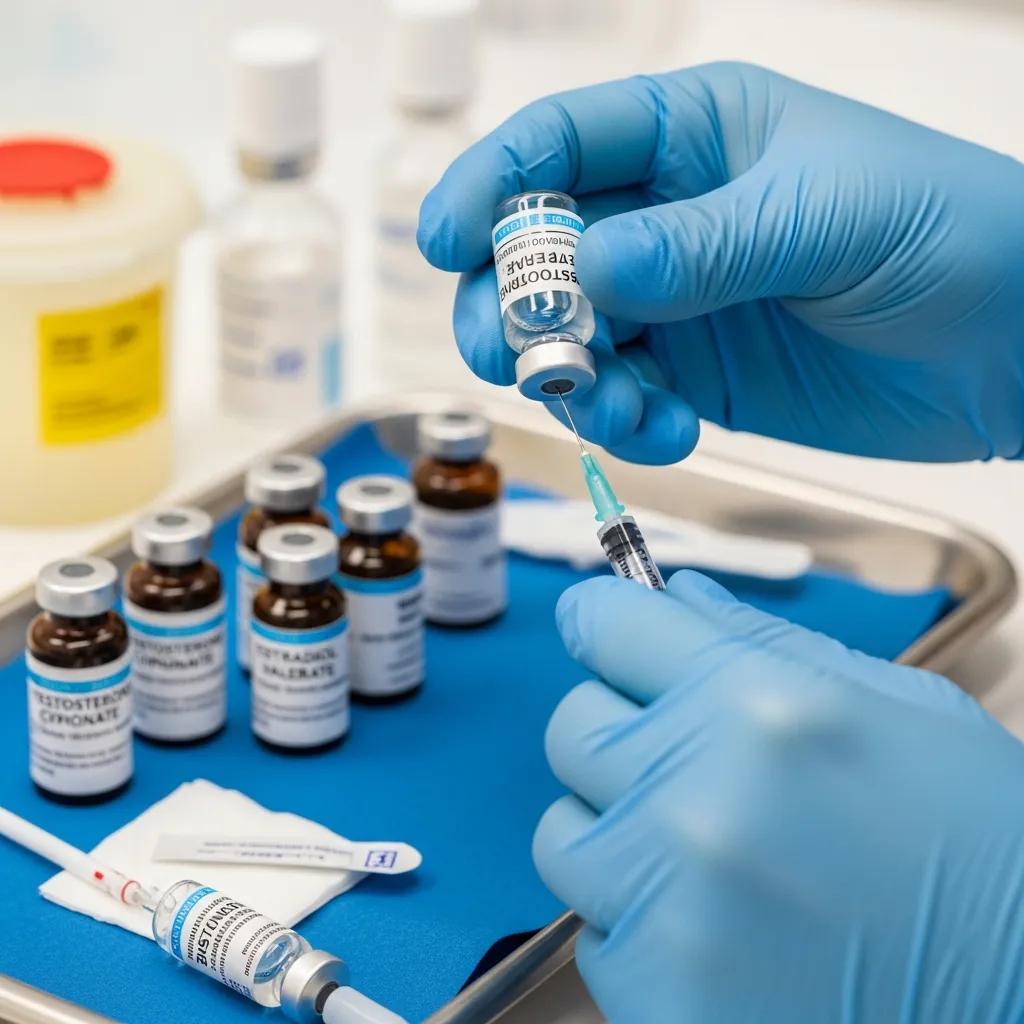
Affirming hormone therapy is a cornerstone of gender-affirming care, providing significant physical and psychological benefits for transgender individuals. The administration of hormone therapy must be approached with careful consideration of dosages, protocols, and patient eligibility to ensure safety and effectiveness.
What Are the Recommended Dosages and Protocols for Hormone Therapy?
Recommended dosages for hormone therapy vary based on individual patient needs and goals. For feminizing hormone therapy, typical regimens may include estrogen and anti-androgens, while masculinizing therapy often involves testosterone. Monitoring hormone levels and adjusting dosages as necessary is crucial for optimizing treatment outcomes and minimizing side effects.
Which Eligibility Criteria and Contraindications Should Clinicians Consider?
Clinicians must consider several eligibility criteria and contraindications when prescribing hormone therapy. Factors such as age, medical history, and existing health conditions can influence a patient’s suitability for treatment. It is essential to conduct thorough assessments and provide patients with clear information about potential risks and benefits before initiating hormone therapy.
What Surgical Interventions Are Included in Current Gender-Affirming Care?
Surgical interventions play a vital role in the gender-affirming process for many individuals. These procedures can significantly enhance quality of life and align physical appearance with gender identity. Understanding the various surgical options available is essential for healthcare providers.
What Are the Clinical Best Practices for Transgender Surgical Procedures?
Clinical best practices for transgender surgical procedures emphasize the importance of comprehensive pre-operative assessments, informed consent, and post-operative care. Surgeons should be well-versed in the specific techniques and considerations for each type of surgery, including chest masculinization, breast augmentation, and genital surgeries. Collaboration with mental health professionals is also crucial to ensure that patients are adequately prepared for the emotional aspects of surgical transitions.
How Do Patient Eligibility and Informed Consent Impact Surgical Care?
Patient eligibility and informed consent are critical components of surgical care in gender-affirming procedures. Healthcare providers must ensure that patients fully understand the implications of surgery, including potential risks and expected outcomes. Informed consent processes should be thorough and transparent, allowing patients to make empowered decisions about their care.
How Is Mental Health Support Integrated into Gender-Affirming Care?
Mental health support is an integral part of gender-affirming care, addressing the psychological needs of transgender individuals throughout their transition. This support can significantly enhance overall well-being and treatment outcomes.
What Mental Health Services Are Recommended for Transgender Patients?
Recommended mental health services for transgender patients include individual therapy, support groups, and family counseling. These services aim to provide emotional support, coping strategies, and a safe space for individuals to explore their gender identity. Mental health professionals should be trained in transgender issues to offer culturally competent care.
How Do Multidisciplinary Care Teams Enhance Patient Outcomes?
Multidisciplinary care teams enhance patient outcomes by providing comprehensive support that addresses the various aspects of gender-affirming care. Collaboration among medical providers, mental health professionals, and social workers ensures that patients receive holistic care tailored to their unique needs. This team-based approach fosters better communication and coordination, ultimately leading to improved patient satisfaction and health outcomes.
Furthermore, integrating ethical considerations and multidisciplinary protocols is crucial for robust gender-affirming care.
Ethics & Multidisciplinary Protocols in Gender-Affirming Care
CES in transgender care can involve ethics consultation or moral case deliberation for particular cases; participation in clinical meetings to draw attention to and clarify ethical issues at play; and input into treatment protocol development. To further illustrate how ethics practitioners can contribute to a multidisciplinary approach to gender-affirming care, the authors also provide examples of embedded ethics support in one transgender care center in the USA based on their experiences.
Clinical Ethics Support for Gender-Affirming Care Teams: Reflections from a Scoping Review, 2022
What Legal and Insurance Considerations Affect Access to Gender-Affirming Care?
Legal and insurance considerations play a significant role in determining access to gender-affirming care. Understanding these factors is essential for both healthcare providers and patients.
How Do Insurance Barriers Impact Treatment Accessibility?
Insurance barriers can significantly impact treatment accessibility for transgender individuals. Many insurance plans may not cover gender-affirming procedures or hormone therapy, leading to financial strain and delayed care. Advocacy for comprehensive insurance coverage is crucial to ensure that all individuals can access the necessary treatments without undue burden.
What Are the Current Legal Protections and Challenges in Transgender Healthcare?
Current legal protections for transgender individuals vary by region, with some areas offering robust protections against discrimination in healthcare settings. However, challenges remain, including legislative efforts to restrict access to gender-affirming care. Staying informed about the legal landscape is essential for healthcare providers to advocate effectively for their patients’ rights.
Where Can Patients Find Reliable Resources and Support for Gender-Affirming Care?
Accessing reliable resources and support is vital for individuals navigating gender-affirming care. Patients should be aware of the various options available to them.
What Patient-Centered Narratives and Case Studies Inform Care Decisions?
Patient-centered narratives and case studies can provide valuable insights into the experiences of individuals undergoing gender-affirming care. These stories highlight the importance of personalized treatment and the diverse paths individuals take in their transitions. Sharing these narratives can foster understanding and empathy among healthcare providers and the broader community.
How Do Educational Materials and FAQs Support Informed Consent?
Educational materials and FAQs play a crucial role in supporting informed consent for transgender patients. Providing clear, accessible information about treatment options, potential risks, and expected outcomes empowers patients to make informed decisions about their care. Healthcare providers should ensure that these resources are readily available and tailored to meet the needs of their patients.
